Seizures due to pregnancy related conditions |
. Eclampsia |
. Posterior reversible encephalopathy |
. Amniotic fluid embolism |
. Local Anesthetic toxicity |
. Cerebral venous sinus thrombosis |
. Thrombotic thrombocytopenic purpura |
. Reversible cerebral vasoconstriction syndrome |
. Air embolism |
JSM Clinical Anesthesiology
-
Review ArticleFor the Parturient, All that Seizes is not Eclampsia. A Review of Psychogenic Non-Epileptic Seizures in PregnancyNnamani NP*, Nguyen L, and Sawyer SDepartment of Anesthesiology, University of Texas at Southwestern Medical Center, USA*Corresponding author: Nwamaka Pamela Nnamani MD, MSc, Department of Anesthesiology, and University of Texas at Southwestern Medical Center, 5323 Harry Hines Blvd, Dallas TX 75390, USA, Tel: 214 648-6400; Fax: 214 648-5461; Email: nwamaka411@yahoo.co.ukSubmitted: 19 February 2019; Accepted: 09 April 2019; Published: 19 April 2019
-
Seizures in the peripartum can be challenging to manage. Seizures in pregnancy can be categorized into these three groups: Known seizure disorder such as epilepsy, pregnancy related causes of which eclampsia is the main culprit and new onset seizures due to another non-pregnancy related problem. This classification of peripartum seizures can be helpful to optimize management. This review will focus on psychogenic non-epileptic seizures (PNES) in pregnancy as it has not been well described in the literature. Psychogenic nonepileptic seizures (PNES) are events characterized by movements or behaviors that resemble epileptic seizures but are not accompanied by abnormal cerebral electrical activity. PNES are psychological in nature and are often associated with stress or emotional triggers. The mainstay of treatment for PNES is psychotherapy, particularly manualized cognitive-behavioral therapy, insight-oriented therapy, and mindfulness technique. The treatment of comorbid conditions such as anxiety or depression can also help decrease the incidence of PNES and an improvement in the overall prognosis. Case reports in the literature describe patients who developed PNES during pregnancy, with the presenting symptoms being severe enough to warrant treatment with benzodiazepines, anti-epileptic drugs, barbiturates, opioids, and even intubation for airway protection. We describe two cases that convey the anesthetic management and the medical challenges of these patients to the medical professionals that treat them.Keywords:Psychogenic Seizure; Epilepsy; Obstetric Anesthesiology
-
PNES: Psychogenic Nonepileptic SeizuresSeizures in the peripartum can be challenging to manage. The parturient can be misdiagnosed with eclampsia and the fetus delivered prematurely, on the other hand a diagnosis could be associated with the risk of being placed on potentially teratogenic medication. Seizures in pregnancy can be categorized into these three groups: Known seizure disorder such as epilepsy (Figure 1)[1] which is exacerbated during pregnancy, pregnancy related causes of which eclampsia is the main culprit (Table 1) and new onset seizures due to another non-pregnancy related problem (Table 2). This classification of peripartum seizures can be helpful to optimize management.
-
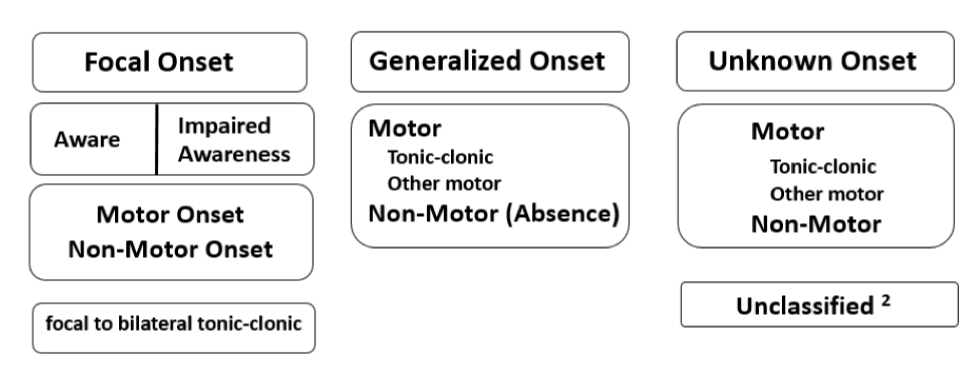 Figure 1: Classification of Epilepsy by International League Against Epilepsy (ILAE)1. View Figure
Figure 1: Classification of Epilepsy by International League Against Epilepsy (ILAE)1. View Figure
-
 Table 1:Seizures associated with pregnancy related conditions. View Table
Table 1:Seizures associated with pregnancy related conditions. View Table
-
 Table 2:Causes of seizures in parturient due to conditions not associated with pregnancy. View Table
Table 2:Causes of seizures in parturient due to conditions not associated with pregnancy. View Table
This review will focus on psychogenic non-epileptic seizures (PNES) in pregnancy as it has not been well described in the literature.Psychogenic nonepileptic seizures (PNES) are events characterized by movements or behaviors that resemble epileptic seizures but are not accompanied by abnormal cerebral electrical activity. PNES are psychological in nature and are often associated with stress or emotional triggers. According to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), PNES is a psychiatric disorder-more specifically; it is a conversion disorder that falls under the category of somatic symptom disorders. It involves the unconscious manifestation of motor or sensory symptoms or deficits that resemble a neurological or medical condition but is not recognized as neurological in nature, not better explained by another medical or mental disorder, and causes clinically significant distress or impairment in functional status [2].The prevalence of PNES in the general population ranges from 2 to 33 cases per 100,000 people [3]. PNES are commonly misdiagnosed as epilepsy and may represent a significant percentage of patients referred to epilepsy centers-up to 20% according to some studies [3,4]. Of patients presenting with intractable seizures, approximately 10% are psychogenic in nature [5]. It is often associated with multiple psychiatric conditions such as major depressive disorders, anxiety or bipolar disorder, post-traumatic stress disorder, and borderline personality traits, and it can be a manifestation of psychological detriment in response to childhood or sexual abuse [6,7]. Roy et al., compared patients with psychogenic seizures with matched cohorts of epileptic patients and found significant differences regarding history of psychiatric disorder, attempted suicide, sexual maladjustment, and current affective syndromes [8]. It is also more commonly seen in patients who have epilepsy or a family history of epilepsy [9]. PNES is more prevalent in females, who represent up to 80% of cases [10]. However, PNES during pregnancy has not been well-described in the literature.The lifetime incidence of non-PNES conversion symptoms has been reported to be as high as 84%, and one study by Lempert et al., reports that other conversion symptoms were present in 60% of patients with PNES [11,12].There are several clinical signs that can aide in diagnosis of psychogenic versus epileptic seizures: gradual onset of seizures, fluctuating course, side-to-side head movements, bilateral asynchronous movements, arching of the back, violent thrashing movements, and vocalizations are all suggestive of psychogenic seizures (Table 3) [1].-
 Table 3:Differences between epileptic tonic clonic and psychogenic non-epileptic seizures. View Table
Table 3:Differences between epileptic tonic clonic and psychogenic non-epileptic seizures. View Table
The diagnosis of PNES can often be challenging, especially in the setting of pregnancy. One of the differential diagnosis that cause significant maternal and fetal morbidity and mortality is eclampsia; a disorder of pregnancy characterized by seizures and associated with hypertension, edema, and proteinuria [13,14]. Brady and Huff describe a case of a female patient at 33 weeks gestation who initially presented with new-onset convulsive activity which was initially treated with benzodiazepines and AEDs despite a probable diagnosis of psychogenic seizures, but with the background of peripheral edema, intermittent hypertension, and proteinuria, eclampsia had not yet been ruled out. Eventually, EEG obtained during the seizure activity prompted the diagnosis of PNES [15].Diagnosis can often be challenging given the often paroxysmal nature of the seizures and the lack of an unequivocal, infallible sign or symptom that definitively distinguishes PNES from an epileptic seizure [16]. The average time to diagnosis of PNES is about 7.2 years [1]. As a consequence, patients with PNES are initially misdiagnosed and are treated for presumed epilepsy; approximately 80% of patients with video-electroencephalogram (v-EEG) confirmed PNES were taking at least one antiepileptic drug (AED) at the time of PNES diagnosis [17]. Unfortunately, these patients tend to utilize significant healthcare resources and suffer more iatrogenic adverse effects than patients with epilepsy [16]. About a tenth of patients presenting with intractable seizures have a psychogenic cause and are often inappropriately treated with potentially toxic anticonvulsant drugs [5]. Further complicating the issue is that patients who have EEG-confirmed epilepsy can have PNES concurrently, and therefore the diagnosis of PNES should not be one of exclusion [9]. Although not without its limitations, v-EEG in concordance with a thorough history and physical is the gold standard for diagnosis of PNES [18].De Toledo et al., reported five cases of recurrent, persistent psychogenic seizures during pregnancy with multiple emergency room visits and continued intake of antiepileptic drugs (AEDs) from various sources, despite the awareness of the psychogenic nature of the seizures and knowledge of the risks associated with AED use during pregnancy [19]. There have also been case reports of patients who developed PNES during pregnancy, with the presenting symptoms being severe enough to warrant treatment with benzodiazepines, AEDs, barbiturates, opioids, and even intubation for airway protection [20,21,22]. PNES can also present as sudden collapse or unresponsiveness, which can often be mistaken for orthostatic hypotension or vasovagal reactions [23,24]. There has been a case reported of PNES as well as pseudo labor in a pregnant patient, eventually diagnosed after fetal fibronectin, fetal non-stress test, and external tocodynamometry were inconsistent with premature labor and uterine contractions [25].29 yo G3P2 at 30 weeks gestation with significant past medical history of seizure disorder (on oxcarbazepine), migraines (on Fioricet prn), Bipolar Disorder, ADHD, and dissociative identity disorder (on Lurasidone, Fluoxetine, Trazodone and Buspirone) presented for management of uncontrolled seizure disorder versus possible pseudo seizures. The patient reported having increased seizure activity over the past 2 weeks with multiple episodes occurring daily. The patient described the seizures as being either tonic-clonic episodes or periods of what she described as “starring spells.” During evaluation by the OB team, the patient had a tonic-clonic episode involving the upper and lower extremities. Immediately after the episode resolved, the patient was alert and oriented to person, place and time; and could answer all questions about her medical history in detail. Neurology team was consulted and they recommended continuing her anticonvulsants and a psychiatry consult. Prior to her evaluation by the psychiatry service, the patient had 2 more episodes of tonic-clonic activity (each lasting approximately 1 minute in duration) and was given 5 mg of Midazolam by the anesthesiology team as well as being loaded with Leviteracetam by the obstetrics team. Again, each of these episodes was followed by no obvious post-ictal state. Shortly after resolution of these episodes the patient signed out against medical advice (AMA) and was lost to follow up.28 yo G8P5A2 with intrauterine pregnancy complicated by asthma, iron deficient anemia and psychogenic non-epileptic seizures (PNES) (diagnosed by video-electroencephalogram (v-EEG) at approximately 17 weeks gestation), she presented at 25 weeks gestation with presumed status epilepticus during pregnancy. According to the patient’s family, she had an episode at home that was described as shaking of her upper and lower extremities in a tonic-clonic manner and tongue biting, but no loss of consciousness. Patient was treated with a total of 25 mg of Ativan (15 mg was given by EMS and an additional 10 mg after arrival to the hospital). In addition, she was given a 3g magnesium load as treatment to prevent eclamptic seizures. The patient had required intubation for inability to protect her airway prior to arrival at our facility. The patient was admitted to the Neurological Intensive Care unit and continuous EEG monitoring was performed. After approximately 24 hours of continuous EEG monitoring, no epileptic form activity could be appreciated. The Psychiatry service was consulted and after another evaluation using video-electroencephalogram (v-EEG), she was diagnosed with PNES. This diagnosis may have been manifested due to Post- Traumatic Stress Disorder (PTSD) and anxiety disorder resulting from the loss of a pregnancy in the past. The patient was taken off all anti-epileptic medications and referred for manualized cognitive behavior therapy in the PNES Clinic.PNES in pregnancy has a complex presentation, diagnostic criteria and subsequent management plan. The differential diagnosis for PNES in pregnancy include: Epilepsy, Eclampsia, metabolic derangements such as hypoglycemia, intracranial occupying lesions and vascular malformations.The two cases described convey the challenges the patients and medical professionals encounter. The first patient left against medical advice likely due to frustration surrounding her diagnosis and treatment plan. The second patient had videoelectroencephalogram (v-EEG) performed twice during her gestation to ensure diagnosis and tailor individualized treatment plan. These two cases show the importance of engaging patients in short and long-term treatment plan.Treatment and Long-Term ManagementAnesthesia management of acute seizure: Individualized psychiatric interventions are the hallmark treatment for psychogenic seizures. Anesthetic management in the seizing parturient should include techniques that involve short acting agents in addition to peri-operative psychological support and constant reassurance for the patient. For acute management of a seizing patient, the patient’s airway should be assessed and managed as deemed necessary. Patient should be oxygenated with a face mask if immediate intubation is not necessary. Vitals signs should be continually monitored. Peripheral intravenous should be placed and a fluid bolus can be commenced. Blood glucose should be checked to rule out the possibility of hypoglycemia. To stop the seizure, benzodiazepines such as midazolam and lorazepam can be titrated. If seizure persists, propofol can be used to help terminate the seizure and for induction to enable intubation and ventilation. Further management should be based on the neurological recommendations.The mainstay of treatment for PNES is psychotherapy, particularly manualized cognitive-behavioral therapy, insightoriented therapy, and mindfulness technique, and the treatment of comorbid conditions such as anxiety or depression can help decrease the incidence of PNES and lead to an improvement in the overall prognosis [26]. The focus should be on treating the underlying trigger while attempting to stabilize the frequency of seizures [27].Long term managementThe long-term outcome in patients with PNES has been shown to be dependent on early diagnosis. McKenzie et al., showed that approximately one third of patients became spell-free after the diagnosis of PNES was made, but 18.7% of patients had a marked increase in the frequency of seizures after diagnosis [29]. Reuber et al., saw that 71% of patients continued to have seizures after diagnosis, 51% were dependent on state benefits, and seizure remission was not a good measure of medical or psychosocial outcome in PNES [30]. Walczak et al., also found that patients continued to have psychosocial issues and be dependent on state benefits despite the diagnosis and cessation of seizures, and 80% of patients had either no change or deterioration in occupational status. Even with complete remission of psychogenic seizures, studies have shown that quality of life does not necessarily improve, and patients can continue to suffer from an unproductive occupational status or significant psychiatric symptoms such as depression, suicidal ideation, and suicide attempts [31].Nwamaka Nnamani wrote a portion of the manuscript and was involved in the management of the 2 cases described. Le Nguyen wrote a portion of the manuscript. Stephen Sawyer wrote a portion of the manuscript. -
-
- Fisher RS, Cross JH, D’Souza C, French JA, Haut SR, Higurashi N, et al. Instruction manual for the ILAE 2017 operational classification of seizure types. Epilepsia. 2017; 58: 531-542.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edn. Arlington, VA: American Psychiatric Association.2013.
- Benbadis SR, Allen HW. An estimate of the prevalence of psychogenic nonepileptic seizures. Seizure. 2000; 9: 280-281.
- Krumholz A. Nonepileptic seizures: diagnosis and management. Neurology. 1999; 53: 76-79.
- Desai BT, Porter RJ, Penry JK. Psychogenic seizures. A study of 42 attacks in six patients, with intensive monitoring. Arch Neurol. 1982; 39: 202-209.
- D’Alessio L, Giagante B, Oddo S, Silva W , Solís P, Consalvo D, et al. Psychiatric disorders in patients with psychogenic non-epileptic seizures, with and without comorbid epilepsy. Seizure. 2006; 15: 333-339.
- Bortz JJ, Prigatano GP, Blum D, Fisher RS. Differential response characteristics in nonepileptic and epileptic seizures patients on a test of verbal learning and memory. Neurology. 1995; 45: 2029-2034.
- Roy. Hysterical seizures. Archives of Neurology. 1979; 36: 447.
- Reuber M. The etiology of psychogenic non-epileptic seizures: toward a biopsychosocial model. Neurol Clin. 2009; 27: 909-924.
- Marchetti RL, Kurcgant D, Gallucci Neto J, Von Bismark MA, Fiore LA. Evaluating patients with suspected nonepileptic psychogenic seizures. J Neuropsychiatry Clin Neurosci. 2009; 21: 292.
- Bowman ES, Markand ON. Psychodynamics and psychiatric diagnoses of pseudoseizure subjects. Am J Psychiatry. 1996; 153: 57-63.
- Lempert T, Schmidt D. Natural history and outcome of psychogenic seizures: a clinical study in 50 patients. J Neurol. 1990; 237: 57-63.
- Sanjay KJ, Alan BE. Psychogenic non-epileptic imitating epileptic seizures. In: Panayiotopoulos CP, editor. Atlas of Epilepsies. London, UK: Springer-Verlag. 2010; 597-609.
- Williams’s obstetrics (24th edn). McGraw-Hill Professional. 2014. ISBN 9780071798938.
- Brady WJ Jr; Huff JS. Pseudotoxemia: new onset psychogenic seizure in third trimester pregnancy. J Emerg Med. 1997; 15: 8.
- Chen DK, Sharma E, LaFrance WC. Psychogenic Non-Epileptic Seizures. Curr Neurol Neurosci Rep. 2017; 17: 71.
- Benbadis SR. How many patients with pseudoseizures receive antiepileptic drugs prior to diagnosis? Eur Neurol. 1999; 41: 114-115.
- Syed TU, LaFrance WC Jr, Kahriman ES. Can semiology predict psychogenic nonepileptic seizures? A prospective study. Ann Neurol. 2011; 69: 997-1004.
- DeToledo JC, Lowe MR, Puig A. Nonepileptic seizures in pregnancy. Neurology. 2000; 55: 120-121.
- Jain U, Jain J, Tiruveedhula V, Sharma A. Psychogenic non-epileptic seizures in a second-trimester pregnant woman with a previous child loss. Prim Care Companion CNS Disord. 2013; 15.
- Valente K, Alessi R. Major stressful life events in pediatric and adult patients with psychogenic nonepileptic seizures. Epilepsy Currents. Conference: 2013 Annual Meeting of the American Epilepsy Society, AES 2013.
- Parry T, Hirsch N. Psychogenic seizures after general anaesthesia. Anaesthesia. 1992; 47: 534.
- Jones SG, O’ Brien TJ, Adams SJ, Mocellin R, Kilpatrick CJ, Yerra R, et al. Clinical characteristics and outcome in patients with psychogenic nonepileptic seizures. Psychosom Med. 2010; 72: 487-497.
- Devireddy VK, Sharma A. A case of psychogenic non-epileptic seizures, unresponsive type, in pregnancy. Prim Care Companion CNS Disord. 2014; 16.
- Carlson RH Jr, Caplan JP. Pseudolabor born out of psychogenic nonepileptic seizures: a case report of multisymptom conversion disorder. Psychosomatics. 2011; 52: 455-458.
- Lesser RP. Treatment and Outcome of Psychogenic Nonepileptic Seizures. Epilepsy Curr. 2003; 198-200.
- Goldstein LH, Chalder T, Chigwedere C, Khondoker MR, Moriarty J, Toone BK, et al. Cognitive-behavioral therapy for psychogenic nonepileptic seizures: a pilot RCT. Neurology. 2010; 74: 1986-1994.
- McKenzie P, Oto M, Russell A, Pelosi A, Duncan R. Early outcomes and predictors in 260 patients with psychogenic nonepileptic attacks. Neurology. 2010; 74: 64-69.
- Reuber M, Pukrop R, Bauer J, Helmstaedter C, Tessendorf N, Elger CE. Outcome in psychogenic nonepileptic seizures: 1 to 10-year follow-up in 164 patients. Ann Neurol. 2003; 53: 305-311.
- Quigg M, Armstrong RF, Farace E, Fountain NB. Quality of life outcome is associated with cessation rather than reduction of psychogenic nonepileptic seizures. Epilepsy Behav. 2002; 3: 455-459.
- Ettinger AB, Devinsky O, Weisbrot DM, Ramakrishna RK, Goyal A. A comprehensive profile of clinical, psychiatric, and psychosocial characteristics of patients with psychogenic nonepileptic seizures. Epilepsia. 1999; 40: 1292-1298.